Right now there is nothing HOTTER and more talked about but also misunderstood, as “gut health”.
My name is Dr. Marc, and today I’m sharing the ‘Nutrition Coach’s Guide to Gut Health.’
If you’re a nutrition coach then delivering better, life-changing results for your clients might come down to what’s going on in the gut, so let’s dive in.
Overview of the Gut Microbiome
I’m sure you’ve noticed it, you can’t scroll 20 seconds on social media without coming across something gut health-related.
There’s a reason why gut health is popular—the gut or gastrointestinal tract is a large group of organs, starting at your mouth, extending all the way to your anus, responsible for digesting food, absorbing nutrients and getting rid of all the waste.
For anyone with an interest in nutrition, this is an important part of the body to study.
But it gets even cooler. The gut is home to over 100 trillion bacteria, both good and bad, living inside the gastrointestinal system.
You’re actually made up of more bacteria than you are human.
Collectively these bacteria are called the “gut microbiota” and they have a profound impact on health, disease and many of the goals our clients want to achieve, like weight balance, improved energy and immunity.
And although this research is relatively new, there seems to be a strong link between what’s going on in your gut and many common diseases.
NOW, some nutrition coaches do have a bad habit of getting a little ahead of the research.
Suggesting things that don’t have tons of evidence or solving problems that aren’t really there.
You may not know this but I did some of my Ph.D. research in the area of nutritional biomarkers in chronic intestinal disease.
I studied under some of the smartest gut doctors in the country, treating some of the sickest patients, and you may be surprised to know that none of them suggested the things you see nutrition coaches on YouTube, TikTok, or Instagram suggesting.
These doctors aren’t out of touch, there just isn’t much evidence to support them yet.
BUT, with that being said gut health is a promising area of study, with a growing body of evidence that clearly shows the influence on health, so today we’re going to dive into that.
But before we start, we need to bring it back.
Let’s go over the human Gastrointestinal System.
Want to Learn More?
Learn more about how to help improve your client's gut health in this video.
Watch Now >>Overview of the Gastrointestinal System
If we want to know where things can go wrong with our guts, we first need to understand how they work.
Our digestive system consists of many different components that help break down food, absorb nutrients and get rid of waste.
Let’s go through the journey of how food travels in our digestive system, from when it enters our mouths all the way to when it gets excreted.
Now under normal conditions, digestion does take an extended period of time, anywhere between 24 to 72 hours to complete the process.
To start this process, we begin at the mouth, where food enters and becomes physically broken down by chewing.
Enzymes in our mouths also chemically break down complex sugar units into simpler sugar units.
Next, it travels down the esophagus and enters the stomach.
The stomach functions to both physically and chemically digest the food. The stomach walls actually have muscles that churn and break down the food, along with acid that breaks down the food components.
The next step for the partially digested food is to enter the small intestine.
The small intestine is a powerhouse for digestion and absorption. It contains many enzymes to help further break down the food.
The small intestine lining is covered with small finger-like projections, called villi and microvilli.
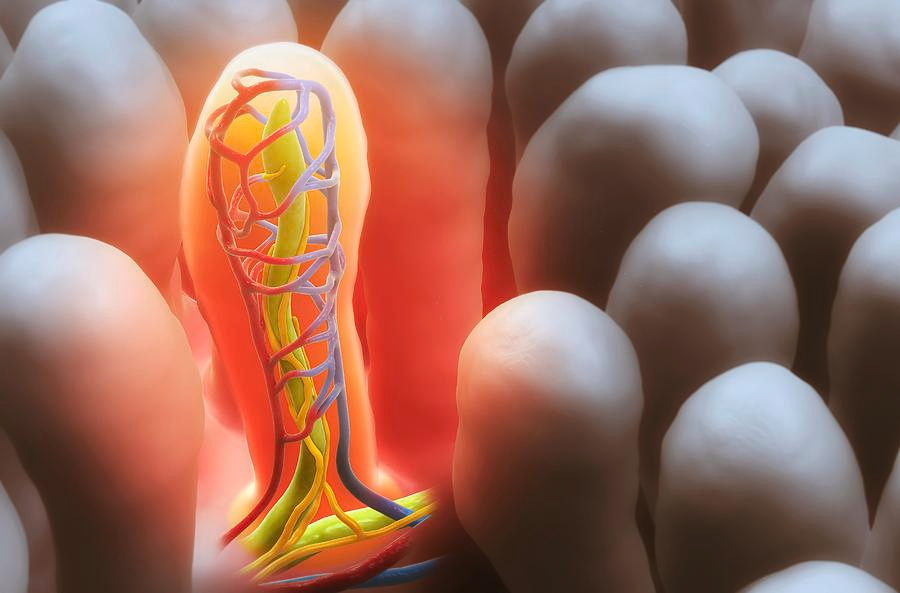
These components help to increase the surface area available for nutrient absorption.
Making the small intestine, the major site for enzymatic digestion and nutrient absorption.
Digested components not absorbed here in the small intestine will make their way to the large intestine (also called your colon).
To put the timing in perspective, undigested food doesn’t get to the colon for 6-8 hours after eating.
Here's where things get really cool for gut health.
Traditionally, we thought of the large intestine as a pathway for waste. This is where additional water was absorbed and feces was formed for excretion.
But research has revealed so much more about our large intestines, specifically the bacteria that live there.
For example, the bacteria in our guts actually ferment fibre to short-chain fatty acids, that our colon cells use for energy.
(Going back to my Ph.D. work I actually did a lot of analysis on short-chain fatty acid production in IBD patients. I won’t bore you with the details, but one thing I do remember is that the short-chain fatty acids smelled a lot like a wet golden retriever.)
There have been some amino acid products that contain them that smell the same.
Anyways, our intestines are home to trillions of microbes that make up what we call the gut microbiome.
There is increasing evidence to show that our gut microbiome can impact beyond our gut health, such as immunity and the risk for chronic disease.
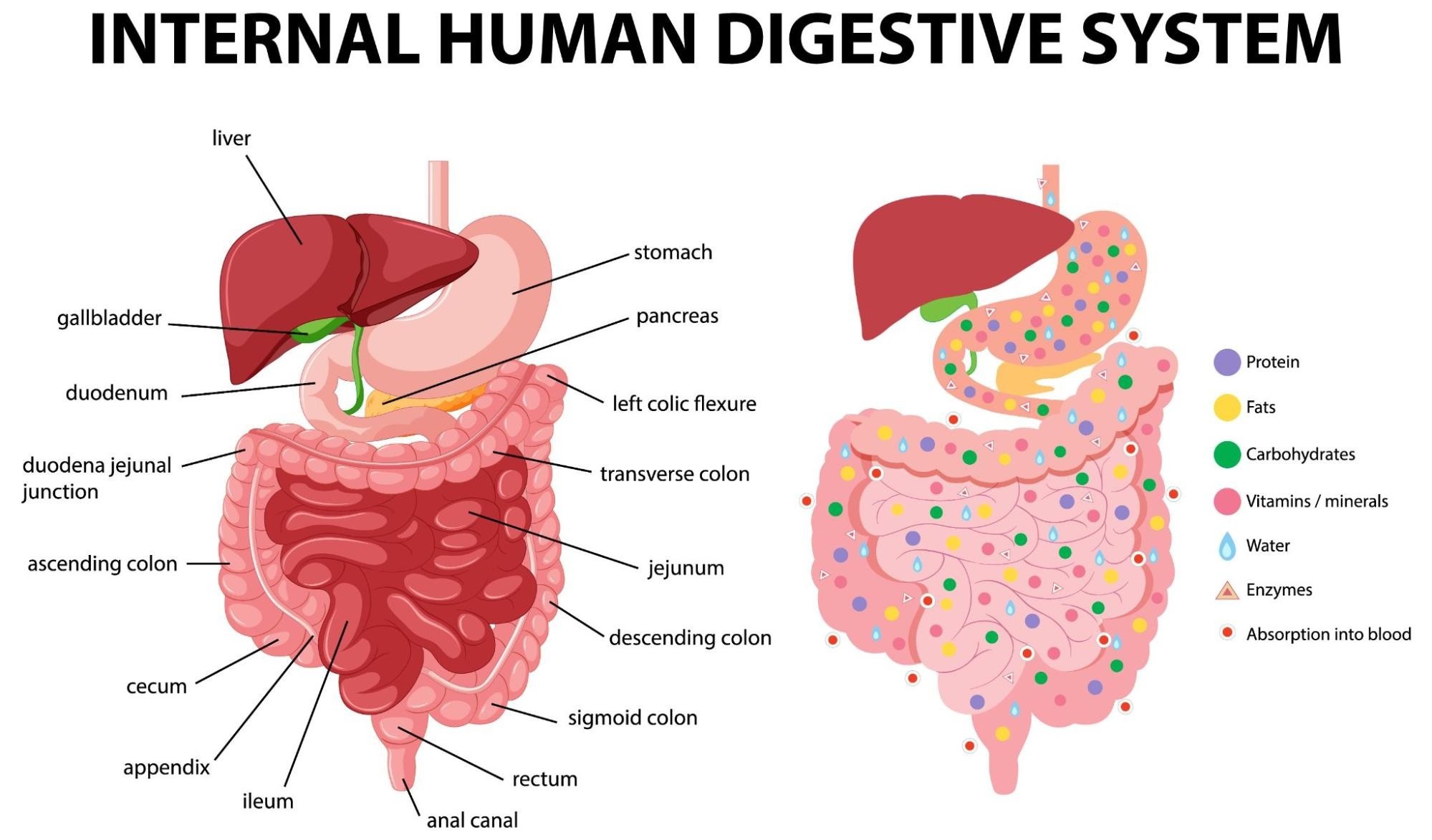
So obviously gut health is important. But what do we really know about it?
But how do you define a “healthy” or “unhealthy” gut?
Well considering the role and function of the gastrointestinal tract.
Our guts must be able to normally break down and absorb nutrients. Without causing excess bloating or gas.
When functioning properly we should be producing anywhere from 3 bowel movements per day or 3 bowel movements per week. Obviously, this is a wide range, but most “healthy guts’ will follow a pattern.
And finally, a healthy gut has a balanced and diverse gut microbiota.
When this is out of whack, our guts can experience “dysbiosis”, which is an imbalance in the types of bacteria in the gut.
Either you have less beneficial bacteria, too much harmful bacteria, or a lack of diversity
When this happens you’re more likely to experience chronic GI symptoms like gas, bloating, constipation, and diarrhea.
Creating the environment for a healthy gut to thrive means avoiding dysbiosis—dysfunction between the gut bacteria and body.
As you can see, most of what influences a healthy gut comes down to the bacteria that live there.
So we need to understand what influences these bacteria to maintain a healthy gut. But what matters most?
Research has shown a diet higher in fibre compared to lower fibre, higher fat and sugar influences the bacteria profile of the gut.
Other factors such as prescription antibiotics and pre-and probiotics (which we’ll detail more later in the video) can influence our gut microbiota.
What we’re going to learn next is what science says about what can be done to influence our gut health.
A few notes: with all the exciting research being done in this field, we need to remain mindful that the evidence is quite limited.
This makes sense, given how new this area of research is.
And although the health of our gut may have implications on our hormones, body weight and even mental health, it’s important to be skeptical of claims that may be too good to be true.
BUT, since nutrition coaches work with so many clients that want body composition changes, what does the science say about gut health and body weight?
There is emerging research on the relationship between our gut microbiome and obesity.
Although preliminary, there seems to be a difference in the bacterial profile between obese and normal-weight individuals
AND those who are overweight have an increased ability to derive energy from food than the gut microbiome of lean.
As well, research from animal studies shows a disruption or a change in the gut microbiome that may be linked to obesity.
There seems to be a link here, but the research is preliminary.
Post this. Get Clients.
Get new nutrition clients on Instagram in just 10-minutes a day using this simple script.
Download >>IBD, IBS and gut symptoms
Now, I do want to contrast what we consider an “unhealthy” gut with the actual disease of the Gastrointestinal tract.
When the gut becomes unhealthy it can experience chronic symptoms like abdominal cramping, diarrhea, gas, indigestion and sometimes pain.
These are the same symptoms that people with Irritable Bowel Syndrome (IBS) will experience chronically.
But there is a big difference between these two situations and Inflammatory Bowel Disease (IBD), which is described as chronic inflammation and sores in the digestive tract.
The two disorders that fall in this category include Crohn’s disease and ulcerative colitis.
And although people with IBD experience abdominal cramping, diarrhea, gas and abdominal pain, symptoms that overlap with “unhealthy gut” or Irritable Bowel Syndrome (IBS), they have visual inflammation that can be seen through endoscopy or colonoscopy.
Which also can cause blood in the stool and serious abdominal pain. These are completely different things.
You may remember my case study with Arlene, she has Crohn’s disease. <LINK TO OTHER ARTICLE>
The management of this type of situation, which is a chronic disease, should be managed by a medical professional.
NOW, We all have experienced gas and bloating to some extent.
These are indications of normal processes during digestion
Certain foods are known to cause an increase in flatulence in some people.
These are pretty individual, without any hard guidelines on what can cause it from person to person.
Healthy foods like broccoli, cauliflower, and beans, have carbohydrates that are digested by the bacteria in our large intestine and can cause excess gas and bloating.
The same foods that improve gut health in some people, can cause gut symptoms in others.
But, when symptoms of an “unhealthy” gut persist for too long, here is what the evidence suggests can help manage it: I’m going to introduce what we know in three categories, strong evidence, neutral evidence and weak evidence.
The Evidence
Strong Evidence
We can’t talk about gut health without discussing dietary fibre.
Fibre is vital for overall health, but it also plays an essential role in the health of our gut.
Our digestive system does not break down dietary fibre; instead, it is metabolized by our gut bacteria.
There is strong evidence to suggest that fibre can have a significant impact on the diversity of our gut microbiome.
Most people should be consuming 14 g of fibre per 1000 kcal of food per day.
Varying sources of soluble fibre (good for lowering cholesterol and blood sugar) and insoluble fibre (adding bulk to bowel movements).
Individuals lacking fibre in their diet show a reduction in the variety of their gut microbiome.
Before someone tries ANYTHING else to improve their gut health, they need to make sure they are eating enough fibre.
Prioritizing fibre-containing foods, like whole grain products, fruits, vegetables, beans, legumes, and nuts and seeds make it easy to reach optimal fibre levels.
Hydration also plays an important role in managing gut health. Staying hydrated may prevent constipation, so a good target for most clients to aim for is 3.7 litres of fluid for adult men, and 2.7 litres of fluid for adult females,
Additionally, a recent study found hydration was linked to increased diversity of bacteria in the gut, although it also indicated the source of water matters.
A sometimes forgotten and perhaps understated aspect of GI health is stress management.
There is a strong connection between the brain and our digestive system. This connection is often referred to as the “brain-gut axis.”
Have you ever noticed that nervous feeling in your stomach? That is due to the work of the nerve cells that line our digestive tract.
When you get too stressed, especially for long periods of time this can impact digestion, causing gas in the short term but even chronic gut issues in the long term.
Stress affects the body. American Psychological Association.
Fibre, hydration and stress are the first lines of defence against poor gut health.
Next, we have strategies with neutral evidence. Keep in mind we may quite, in fact, learn more about these and they end up playing a more important role in gut health, but for now, they are “nice to try” instead of need to try.
Neutral Evidence (Pre and Probiotics)
You may have heard of the terms pre and probiotics when it comes to gut health.
Probiotics are live bacteria that help colonize the gut, while prebiotics is the food these bacteria need to thrive.
Foods that contain probiotics that may be helpful to improve gut health are fermented foods like yogurt, sauerkraut, kimchi and kefir, which help colonize the gut with helpful bacteria,
The evidence on their effectiveness is mixed though.
It seems that probiotics can be beneficial in reducing symptoms of specific diseases such as IBS and IBD.
However, we have weak evidence to show their effectiveness in mood disorders (depression, etc.) and weight loss.
For now, consuming fermented foods that contribute to a healthy diet makes sense, but I wouldn’t go out of my way to take a probiotic supplement.
There’s just not enough evidence to suggest their use in healthy people at this point.
For prebiotics, although I wouldn’t go out of my way to suggest any specific prebiotic foods, eating fibre-containing foods with fibre requirements is always smart.
Although probiotics and prebiotics may not the difference maker for gut health, they are usually part of healthy food or safe for people to take, so if someone wants to take them, that wouldn’t be the hill I would die on.
BUT with that being said, what has Limited Evidence or is mostly BS for improving gut health?
Limited Evidence And BS
Food sensitivity tests
There can be a lot of misinformation regarding food sensitivity tests and their impact on gut health, inflammation and overall well-being in general.
Many of these tests are at-home kits that use markers from blood tests and claim to provide a list of foods you may be “sensitive to”.
It is important to note the differences between a food allergy, intolerance and sensitivity.
For instance, food allergies happen when food causes our immune system to react by producing antibodies. Symptoms such as shortness of breath and a skin rash may arise.
Food intolerance is when our bodies have trouble digesting food due to lacking a particular enzyme. An example would be lactose intolerance, which results from the inability to digest lactose.
While food sensitivity is not a medical diagnosis and is sometimes an umbrella term to describe a food intolerance or allergy, it is important to know that there is little evidence behind food sensitivity tests.
Food allergy tests use immunoglobulin E (IgE) to detect a proper immune response to a food.
In comparison, food sensitivity tests look for immunoglobulin G (IgG). There is limited evidence to suggest that IgG is a reliable method to detect food allergies or intolerances.
We know that measuring IgG is not specific since it simply shows that the individual has had past exposure to the food item.
This causes fear more than anything else.
Recently, you may also have seen at-home testing kits that claim to sequence the bacterial genome in your gut microbiome through fecal samples. Many of these testing kits claim that you can tailor your diet and nutrition based on your unique gut microbiome; however, there is limited evidence to support this claim.
While it may be neat to know this information, we’re not at the point where we can give suggestions to our clients based on it. Evidence shows that we can also guess the bacterial profile of your gut microbiome based on an individual's diet to some extent.
That’s it, folks, gut health is a scorching topic and for good reason. We’re learning more about it all the time and the impact it has on our overall health. I hope you found this information and the strategies provided useful for you and your clients.
As great as all these tips are, if you’re really serious about starting a nutrition coaching business then the next thing you’re going to want to do is to check out the video I have linked below. Now that you have a better understanding of gut health, learn about the pros and cons of the Carnivore Diet.
So make sure to check it out now and I’ll talk to you next time
Is the Carnivore Diet Healthy?
The overview of what the carnivore diet is, the benefits of all animal-based protein, and the drawbacks of excluding plant sources of food.
Video >>




